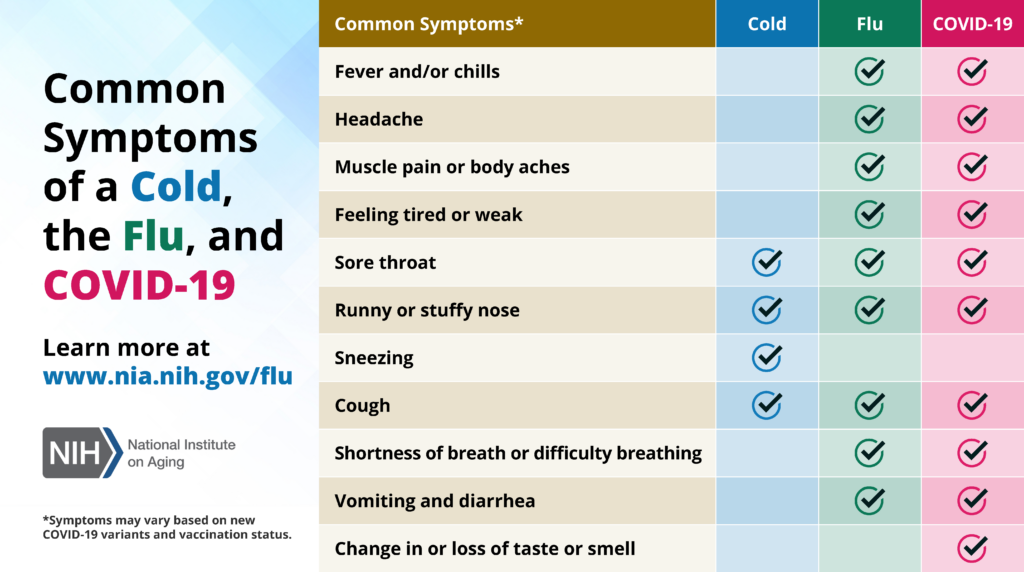
Providing care for an older adult can be overwhelming, especially at the beginning. On this page, you will find answers to frequently asked questions about caregiving.
Click on each of the expandable sections below to see the answer to each question and links to other resources.
I’m new to caregiving. Where do I start?
If you have never been a caregiver before, it may feel daunting at first. There might be tasks to organize, new medical terms to learn, and schedules to coordinate. Start by thinking about:
If you don’t live nearby, you can learn about ways to provide support and assistance as a long-distance caregiver.
How can I find a caregiver support group?
Caregiver support groups (online or in-person) are a great way to connect with people who understand what you’re going through.
Your doctor or faith community may be able to help you find the right support group. You can also reach out to your local senior center, state office on aging or social services office, or local Area Agency on Aging for information about support groups. The Family Caregiver Alliance and the Caregiver Action Network offer online and in-person settings for caregivers to connect with one another.
Caring for an older adult can be both rewarding and challenging. Learn about more ways you can take care of yourself as a caregiver.
How do I help an older adult plan for the future?
You may need to help your loved one plan for the future by preparing important documents and storing them in a safe place. Learn how to get their affairs in order, which includes locating and organizing legal, financial, and personal records.
Depending on your loved one’s medical needs, you may need to help them prepare advance directives, which are legal documents that provide instructions for medical care if a person cannot communicate their own wishes. Get tips and worksheets to help you discuss advance care planning with your loved one.
How do I choose a long-term care facility?
When an older person needs more help than family and friends can provide, it may be time to consider moving to a residential (live-in) facility, such as assisted living or a nursing home. Choosing a place to live for long-term care is a big decision. It can be hard to know where to start.
Before you choose a long-term care facility for your loved one, consider their needs and wants. Talk to friends and family in your area and call and visit different facilities. Ask questions during your visit and ask for information about costs and payment options.
I’m overwhelmed and exhausted. How can I get a break from caregiving?
Taking care of a family member is hard work. But taking care of yourself is important, too. All caregivers need a break from time to time. Don’t wait until you’re completely overwhelmed to seek help from family, friends, or professional services.
Accepting help from others isn’t always easy. You may worry about being a burden, or you may feel uncomfortable admitting that you can’t do it all yourself. Get tips for how to ask family members or friends for help.
Respite care may also be an option. Respite care provides short-term relief for primary caregivers, giving them time to rest, travel, or spend time with other family and friends. The care may last anywhere from a few hours to several weeks at a time. Respite care can take place at home, in a health care facility, or at an adult day care center.
How do I make an older person’s home safer?
There are a variety of ways to make an older adult’s surroundings safer and easier to manage. Go through the house room by room to identify potential problems and safety issues. First, correct any immediate dangers, such as loose stair railings and poor lighting, and then work on other ways to ensure the person will be as safe as possible at home.
Download this Home Safety Checklist for room-by-room suggestions to help you identify and remove hazards around the house.
Are you worried that making changes might be expensive? You may be able to get help paying for repairs and safety updates to an older adult’s home. Check with your state housing finance agency, social services department, community development groups, or the federal government for financial aid programs and discounts. You can also contact the Eldercare Locator for help finding resources.
To learn more, please visit https://www.nia.nih.gov/health/caregiving/frequently-asked-questions-about-caregiving.